Seborrheic dermatitis is a chronic inflammatory skin condition characterized by persistent redness, flaking, and epidermal irritation. While frequently mistaken for common dandruff or psoriasis, managing this condition requires a specialized clinical approach to stabilize the skin barrier and prevent recurrent flare-ups without relying on aggressive chemical agents.

Common Symptoms of Seborrheic Dermatitis:
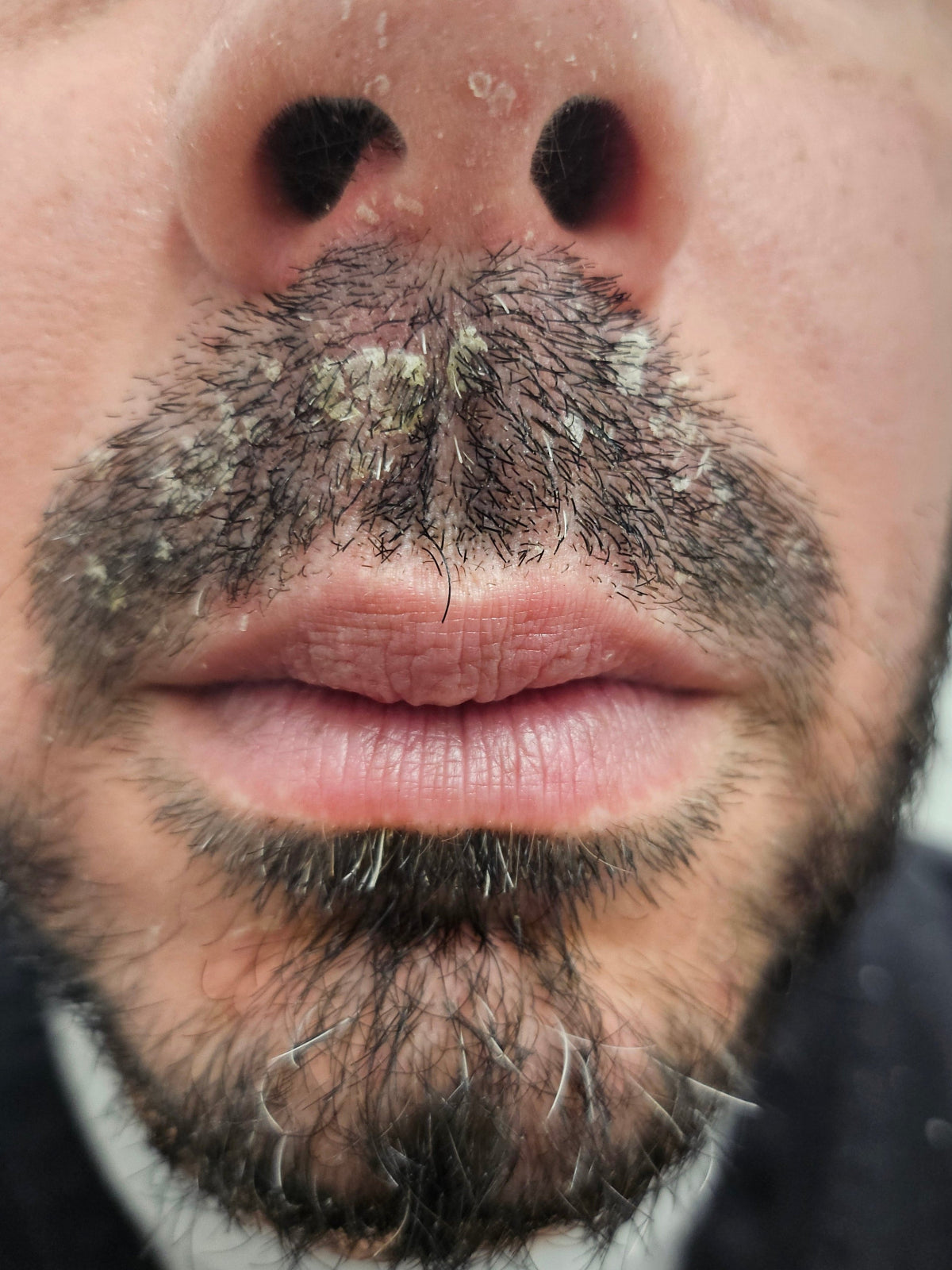
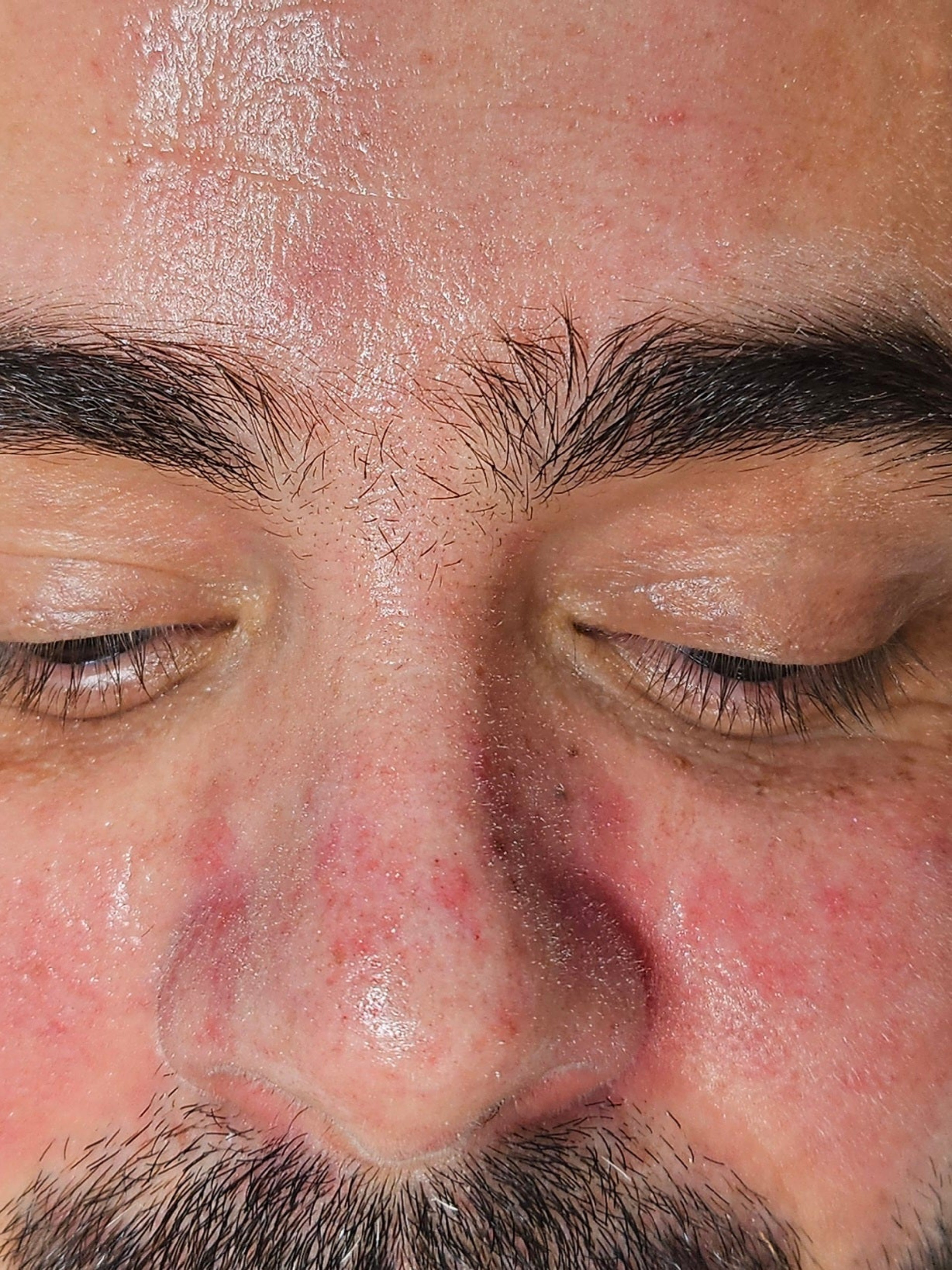
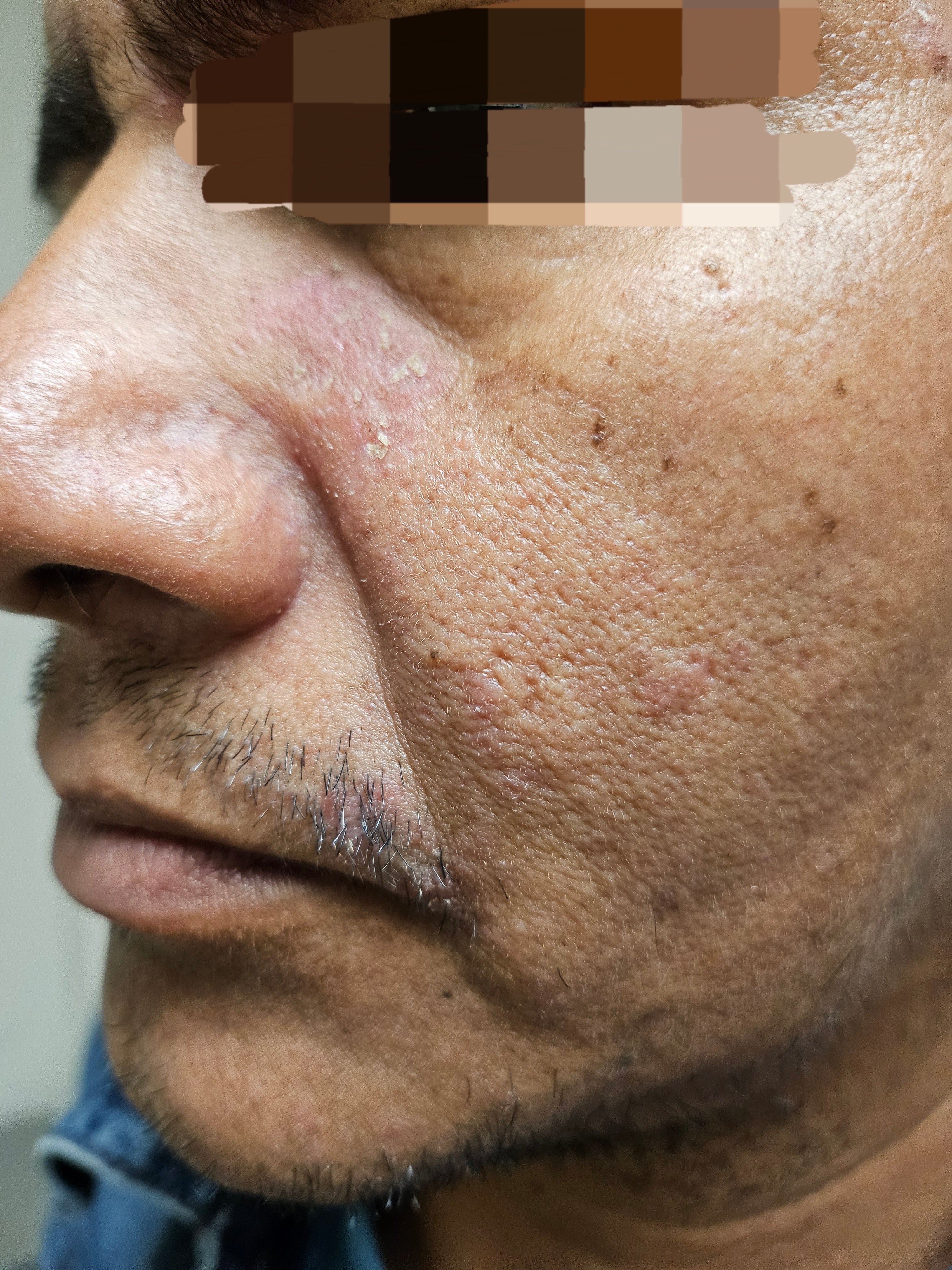
✔ Persistent, adherent flakes localized along the hairline, eyebrows, or facial hair regions.
✔ Inflamed, reddened plaques exhibiting a distinct greasy or yellowish scaly appearance.
✔ Intense itching or a localized burning sensation during active inflammatory phases.
✔ Significant epidermal crusting, particularly in advanced or unmanaged cases.
✔ Elevated reactivity and sensitivity when exposed to standard commercial cosmetic formulations.
What areas does seborrheic dermatitis affect?
The topography of this condition correlates directly with regions of the body exhibiting the highest density of sebaceous glands. These zones are prone to significant lipid accumulation, creating optimal conditions for microbial proliferation.
| Target Zone | Clinical Manifestation | Sebum Concentration |
|---|---|---|
| Deep follicular oil production. Thick yellowish adherent scales and intense chronic pruritus. |
Sebum Saturation: Maximum
|
|
| Surface erythema in the T-Zone and nasolabial folds. Presentation of fine, greasy flaking. |
Sebum Saturation: High
|
|
| Localized presternal petaloid patches. Erythematous base with moderate lipid presence. |
Sebum Saturation: Moderate
|
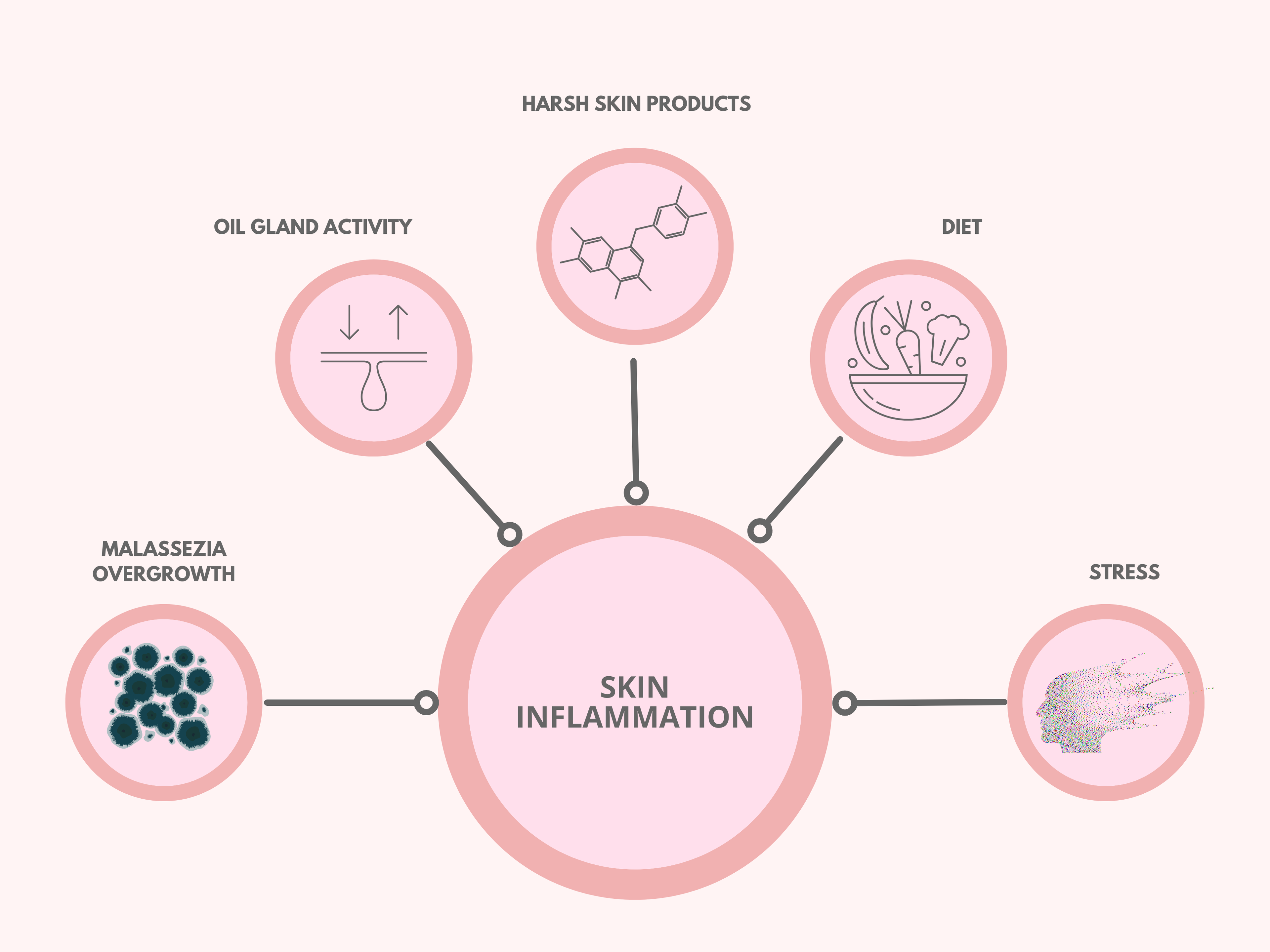
The Root Cause
The development of this condition is multifactorial, involving a complex interplay of genetic predisposition, hormonal fluctuations, and compromised skin defense mechanisms. Elevated psychological stress and the application of stripping topical agents further degrade the skin's protective barrier. When this structural integrity fails, excessive oil production provides a lipid-rich environment that disrupts the natural microbiome, leading to chronic localized inflammation.
The Role of Malassezia Yeast
Understanding the tiny fungus that lives on everyone's skin
The Pathway to Inflammation
A Normal Skin Resident
Malassezia is not a foreign invader, but a natural component of the human cutaneous ecosystem. This microscopic yeast colonizes the skin of approximately 90% of adults, coexisting peacefully with other microorganisms. It has evolved alongside us for millennia without inherently causing adverse dermatological reactions.
When Overgrowth Occurs
Complications emerge only when this delicate microbial balance is disrupted. Clinical triggers such as excessive sebum production, high humidity, hormonal fluctuations, or immunosuppression create an optimal breeding ground. These variables allow the yeast to proliferate exponentially beyond manageable levels.
The Sebum Connection
Biologically, Malassezia is strictly lipophilic, meaning it thrives on lipids. The yeast actively feeds on triglycerides found in human sebum, breaking them down into reactive free fatty acids. The accumulation of these metabolic byproducts penetrates the epidermal barrier, severely irritating the tissue and triggering an immune response.
Why Oily Areas Are Affected
The distribution of seborrheic dermatitis is directly linked to human glandular anatomy. The scalp, central face, and upper chest harbor the highest density of active sebaceous glands. A higher volume of lipid secretion provides a larger food source, inevitably leading to a higher concentration of yeast in these specific anatomical zones.
Key Takeaway
Malassezia isn't the enemy—imbalance is. Managing oil production and maintaining skin barrier health keeps this natural resident in check.
How to Avoid Flare-Ups
Achieving long-term remission demands a rigorous and scientifically grounded skincare regimen. Implementing the following daily protocols can significantly mitigate the frequency and severity of inflammatory episodes:
pH-Balanced Cleansing
Cleanse affected regions exclusively with sulfate-free dermatological formulations to preserve the acid mantle.
Avoid Micro-Trauma
Abstain from mechanical exfoliation or scratching to prevent micro-abrasions and secondary bacterial infections.
Cortisol Regulation
Implement stress-reduction strategies to regulate cortisol levels, which directly influence sebaceous activity.
Barrier Hydration
Apply non-comedogenic, barrier-repairing moisturizers that hydrate without contributing to lipid overload.
Environmental Control
Minimize prolonged exposure to extreme humidity or situations causing excessive perspiration.
Epicderma Support
Integrate specialized skin nourishment for barrier repair to maintain a resilient and balanced cutaneous ecosystem.
Finding Balance: A Natural Approach
At Epicderma, we focus on gentle, effective solutions that target SebDerm at the source—without the side effects of conventional treatments. Are you ready to take control of your skin with nature-powered relief?


